Digital pathology is no longer a future ambition. It is an operational reality reshaping how laboratories and health systems diagnose, collaborate, and innovate. After attending the Digital Pathology Association (DPA) Conference in San Diego this year, I left energized by the level of innovation and the thoughtful conversations surrounding digital pathology implementation. Whether discussions involved academic medical centers, community hospitals, or industry partners, one message remained consistent: the promise of digital pathology is undeniable, but successful implementation requires thoughtful navigation of both technical and cultural change.
Digital transformation is rarely a single-step process. Instead, it is a coordinated effort that depends on strategic planning, interdisciplinary collaboration, and adaptability. Histotechnologists must adjust slide preparation workflows, information technology teams must create secure and scalable systems, administrative leaders must allocate resources, and pathologists must integrate new tools into diagnostic practice. When these diverse roles work in alignment, implementation becomes not just possible, but sustainable.
Below are several commonly discussed challenges from the meeting, along with practical strategies that may help laboratories transition more confidently into a digital environment.
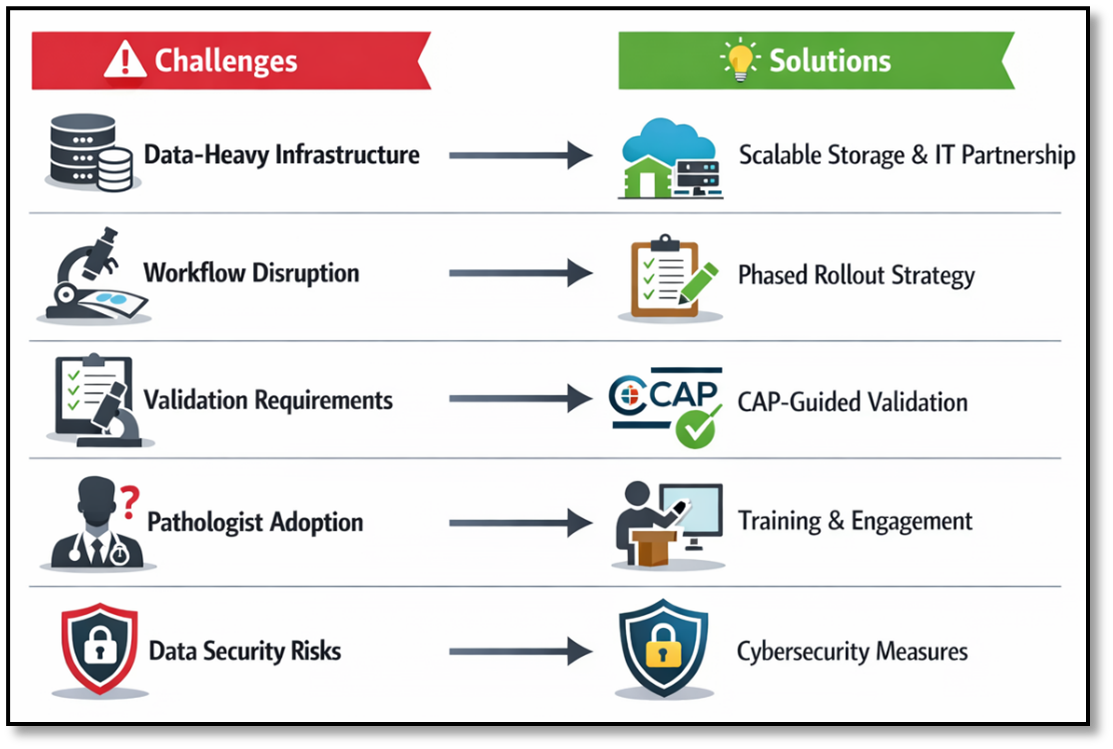
Building Technical Infrastructure for a Data-Heavy Future
Challenge: Whole slide imaging (WSI) generates enormous data volumes that can quickly exceed traditional storage capacity and place significant strain on IT infrastructure.
Practical Resolution: A strong infrastructure lays the groundwork for downstream success in digital pathology. Early and continuous partnership between pathology departments and IT professionals is essential. Designing a scalable storage strategy, such as a hybrid model combining local and cloud-based solutions, provides flexibility while helping control long-term costs. Additionally, adopting DICOM standards and vendor-neutral archives supports interoperability and helps future-proof systems as technology evolves.
Integrating Digital Tools Without Disrupting Workflow
Challenge: Transitioning from glass slides to WSI can disrupt well-established processes, particularly in high-volume laboratories or systems operating across multiple sites.
Practical Resolution: A phased rollout allows teams to adapt gradually while minimizing operational friction. Many institutions benefit from beginning with targeted use cases such as tumor boards, frozen sections, or consultative cases. These early applications provide valuable opportunities to identify workflow gaps, refine processes, and build user confidence.
Importantly, feedback should be gathered not only from pathologists but also from histotechnologists, laboratory staff, and operational leadership. Their perspectives can reveal practical insights that improve efficiency and support diagnostic accuracy.
Ensuring Validation and Regulatory Confidence
Challenge: Demonstrating diagnostic concordance between digital platforms and traditional microscopy is essential for regulatory compliance and for developing user trust.
Practical Resolution: Following CAP digital pathology validation guidelines offers a reliable approach. Validating a representative set of cases through both digital and glass slide review helps confirm diagnostic accuracy, while documenting scanner performance and monitor calibration strengthens quality assurance efforts.
When validation is approached as a transparent and collaborative process, it helps to reassure stakeholders that innovation is being implemented responsibly.
Supporting Pathologist Adoption Through Education
Challenge: Even the most advanced systems will struggle if users are hesitant to adopt change. Concerns related to image quality, navigation speed, and workflow changes can slow momentum.
Practical Resolution: Engagement must begin early. Providing hands-on training sessions, enabling side-by-side comparisons, and involving pathologists in system testing can increase familiarity and confidence. Education should emphasize tangible benefits, including remote sign-out capabilities, rapid access to archived slides, quicker consultation between users, and emerging AI-assisted tools. A focus on these aspects can reinforce how digital workflows can enhance, rather than hinder, diagnostic practice.
Protecting Data While Promoting Connectivity
Challenge: As digital slide repositories expand, so does the responsibility to safeguard sensitive data while maintaining seamless communication between systems.
Practical Resolution: Incorporating cybersecurity measures from the outset is imperative. Encryption, role-based access controls, and routine security audits help protect patient information. Selecting platforms that integrate smoothly with the laboratory information system (LIS) further reduces downtime and prevents technical bottlenecks.
Looking Ahead: Digital Transformation as a Human Endeavor
The digital pathology community continues to demonstrate that implementation success depends on far more than scanners and software. It is fundamentally a human endeavor that requires communication, shared vision, and commitment across disciplines.
When pathologists, histotechnologists, IT specialists, administrators, and laboratory teams collaborate effectively, they create workflows that improve diagnostic precision, streamline operations, and open the door to advanced computational pathology.
Digital pathology is transforming not only how we view slides, but how we function as a field. Each successful implementation moves us closer to a fully digital future, one that elevates the practice of pathology and ultimately enhances the care that we deliver to patients.
Author

Sara Niyazi, DO
Pathology Resident Physician
University of South Florida
2025 DAPA Trainee
Please log in to your DPA profile to submit comments